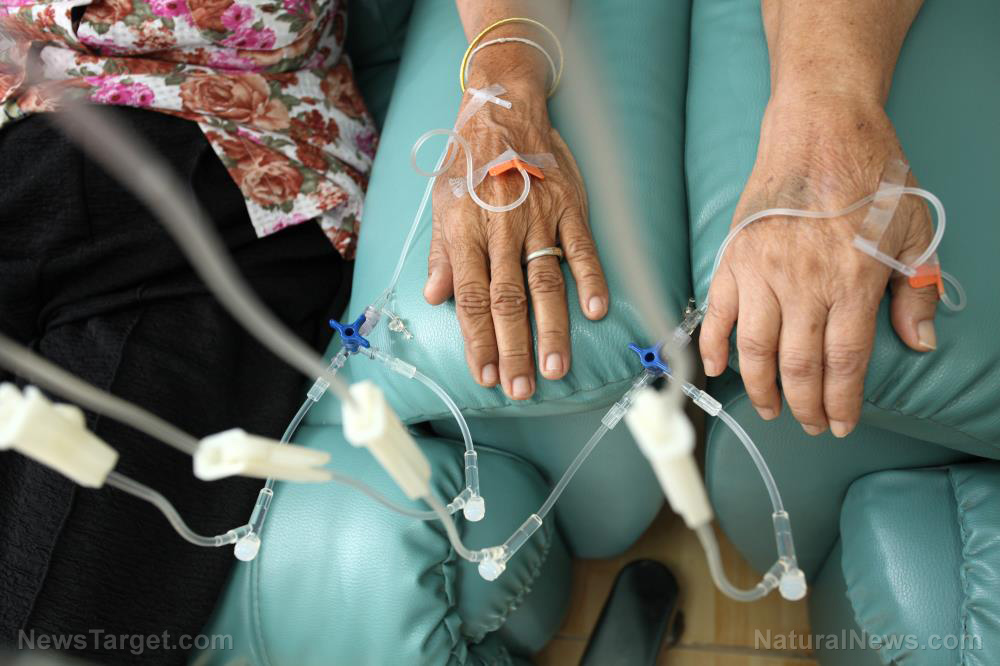
How is death an acceptable side effect of “treatment?” Cancer drug could take out your heart, according to research
01/24/2019 / By Tracey Watson
Multiple myeloma (MM) is a form of cancer that develops in white blood cells called plasma cells. While plasma cells usually form part of the body’s immune defense system, in MM patients, these cells become cancerous and multiply rapidly, causing bone tumors, anemia, recurring infections and kidney failure. Around 30,000 Americans are diagnosed with the condition each year, and it causes approximately 12,500 deaths annually.
The Mayo Clinic notes that not all MM patients require treatment, but for those who do, conventional treatment includes chemotherapy, radiation, and the use of drugs called proteasome inhibitors. The U.S. Food and Drug Administration (FDA) has approved the use of three different proteasome inhibitors, one of which is called Carfilzomib.
Now, a study by researchers from the Abramson Cancer Center of the University of Pennsylvania has warned that the use of Carfilzomib is associated with a dramatic increase in the risk of cardiovascular problems, including hypertension, heart attacks, heart failure and arrhythmia (an abnormal heart rhythm).
The study was published in the journal JAMA Oncology last month.
Proteasomes are protein complexes which have the job of breaking down and eliminating proteins within a cell. Since multiple myeloma requires an increased number of proteasomes to survive, proteasome inhibitors, including Carfilzomib, work by preventing them from doing their job, causing protein to build up in the cells, and leading to cellular death.
While this process in theory kills cancer cells, like all conventional cancer treatments it also causes peripheral damage.
“Like any cancer therapy, the concern with this approach is that it may have an effect on an otherwise healthy part of the body — in this case, the heart,” said Adam J. Waxman, MD, the study’s lead author, and a Hematology Oncology fellow with the University of Pennsylvania’s Perelman School of Medicine.
When the researchers collected data from 24 studies conducted on 2,594 patients between 2007 and 2017, they found that 18.1 percent of the patients who took Carfilzomib experienced a cardiovascular adverse event (CVAE). Of these, 8.2 percent experienced severe, grade 3 events.
The most common CVAEs were hypertension (12.2 percent) and heart failure (4.1 percent). Arrhythmias (2.4 percent) and ischemic events (1.8) — in which there isn’t enough blood flow to the heart leading to the death of heart muscle — were observed less commonly. Researchers also found that higher doses of carfilzomib are associated with higher rates of CVAE, and that carfilzomib was associated with an elevated risk of CVAE compared to control groups who did not receive carfilzomib.
Waxman warned that patients taking these medications should be made aware that they are exposing themselves to an elevated risk of CVAEs.
The study’s findings are particularly disturbing since people who have MM are already more susceptible to CVAEs, as the conditions carry many of the same risk factors, including increased age and obesity. Earlier research found that around 66 percent of MM patients had cardiovascular disease at baseline, with 70 percent going on to experience some form of cardiovascular event within six years.
With this danger in mind, Waxman warned that health practitioners need to tailor their treatment plans carefully when caring for patients with multiple myeloma.
For those with MM who wish to avoid the risk associated with Carfilzomib and other chemical drugs, there is good news: Back in 2013, researchers from Virginia Commonwealth University (VCU) in Richmond reported that, when combined with molecules from the anti-nausea drug thalidomide, the spice turmeric – the active ingredient of which is commonly known as curcumin – is capable of targeting and killing multiple myeloma cells naturally.
“Overall, the combination of the spice and the drug was significantly more potent than either individually, suggesting that this hybrid strategy in drug design could lead to novel compounds with improved biological activities,” said Dr. Steven Grant, M.D., one of the study’s authors. “Enhanced potency, reduced risk of developing drug resistance, improved pharmacokinetic properties, reduced cost and improved patient compliance are just a few of those advantages.”
Sources for this article include:
Tagged Under: